Uterine Fibroid Embolization
Uterine fibroid embolization (UFE, also known as uterine artery embolization UAE) is a procedure performed by an interventional radiologist (IR). The technique involves placing a catheter into the artery and guiding it to the uterus. The IR then injects small particles of plastic (polyvinyl alcohol or PVA) into the artery. The PVA blocks the blood supply feeding the fibroids and this results in embolization. The whole procedure takes about an hour and you are sedated but awake the entire time.
Within minutes after the procedure the fibroids begin dying. Generally, (but not always) there is an overnight stay in the hospital because many women have felt intense abdominal cramping and pain. Post-procedural pain is usually controlled through the use of a combination of narcotics but some IRs have started using epidurals (spinal anesthesia) to block all pelvic region pain for 12 hours or so. Ninety-nine percent (99%) of the women who undergo this procedure go home after only 1 night in the hospital.
Recovery is 1-2 weeks. Most women are up and around within a couple of days. The majority return to work after only 1 week of recovery. I returned to work after 6 days off but probably could have waited and returned after the second week. However, there was no traumatic surgery to recover from, no hormonal whammies from having anything "removed", and no psychological stress involved regarding the removal of the uterus.
|
Post Embolization Syndrome Post embolization syndrome is something that I and many other women have experienced with uterine fibroid embolization. Although most of the immediate side effects or symptoms that are the result of this procedure do not last long, post embolization syndrome can take up to 6 weeks to go away. So what is this syndrome? It consists mostly of menopause-type symptoms, such as hot flashes, a general sense of not feeling well, and nausea. It can be downright annoying and troublesome. As the fibroids die, toxins are released into the blood stream that can cause these symptoms. While the majority of women recover from these symptoms within 1 to 2 weeks post procedure, they have been known to last as long as 6 weeks. CRITICAL NOTE: If any of the symptoms you experience include an ever increasing amount of pain or a rise in fever that does not subside within a short period of time, contact your physician immediately for further evaluation. |
Ideal Patient
The ideal patient for this procedure meets four basic requirements:
- they have fibroids
- the fibroids are symptomatic
- there is no cancer
- future pregnancies are not desired.
Although some interventional radiologists have additional requirements, it is not proven that any of these requirements have a basis in scientific data collected thus far. For instance, one interventional radiologist states that he doesn't accept patients that have a fibroid uterus that has grown above the navel in size -- any fibroid uterus roughly larger than a 16-20 week pregnancy is unacceptable. In his experience, the percentage of shrinkage from this size of fibroid uterus is not significant enough to warrant doing the procedure. However, his experience may include fewer than a dozen patients with fibroids of this size. Collectively, the data simply hasn't been reviewed yet for efficacy of UFE in relationship to size of fibroid uterus. Who knows whether or not his exclusionary patient selection process is valid? Maybe it is. Maybe it isn't.
Still other IRs are turning women away because they are 50 years of age or more. Since the average age of menopause is 51, they've somehow determined that doing nothing and simply waiting out menopause is a more appropriate course to take for these women. Nevermind that 51 is the average age of menopause. (The women in my family didn't hit menopause until they were nearly 60 or so.) Nevermind that the women are bleeding like there's no tomorrow.
Someone needs to tell these docs that the word AVERAGE means there's a span of difference with a low and a high and the numerically totaled and divided middle point is the AVERAGE. Geez.
The average age of menopause is 51, give or take 1 to 15 years. Capiche?
Come on guys. Don't make me draw a bell curve here. Appropriate testing can be done that would determine a little more accurately where a woman is on the spectrum from peri-menopause to post-menopause.
Some additional concerns and considerations might include:
a) the presence of submucosal fibroids which can or should be resected hysteroscopically
b) the presence of pedunculated subserosal fibroids more effectively treated by removing them via myomectomy.
UFE treats all uterine fibroids at the same time and is, therefore, an extremely effective, all encompassing treatment option. However, submucosal fibroids not removed before UFE may infarct once they die and cause the uterus to attempt to get rid of the fibroid. If the fibroid is too large for the uterus to expel, serious infection could result. This can be extremely painful and potentially dangerous. It is important for women with submucosal fibroids to discuss this possibility with their gynecologist and determine how to handle the care of their submucosal fibroids before the UFE.
Pedunculated subserosal fibroids may also infarct and break off from the uterus once they necrotize. This has been known to create a temporarily painful condition treatable with pain medication but, so far, no additional problems have been encountered. Only more time will tell us whether or not this is a complication with additional concerns.
Success, Failures, and Complications
Doctors are currently tracking success and failure of this procedure by two different standards: technical failure and clinical failure. Knowing the difference between these two kinds of failures will give you a better understanding of what the success statistics actually mean to you when you read them. In addition, complications can occur during the procedure which result in injury, a less than desired outcome, or unanticipated results.
Technical Failure Rates
Technical failures currently occur 1-2% of the time and are primarily related to the following items.
- skill of interventional
radiologist
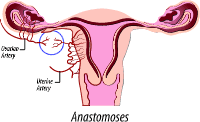
- abnormalities of the uterine artery
- shared blood flow from a single uterine artery and ovarian artery (with both feeding the fibroids) -- a blood flow situation called anastomoses
- use of progestin or GnRH agonists (Lupron) pre-UFE
- any number of additional odd circumstances that present themselves during the procedure.
Clinical Failure Rates
Clinical failure rates are another cup of tea entirely. Typically these have nothing to do with the interventional radiologist and his/her embolization of your artery but rather your own physical response to the embolization. If the embolization is a technical success but the symptoms the fibroids were causing are not significantly or satisfactorily reduced post-UFE, then this is considered a clinical failure. For example, if the fibroids don't shrink "enough" or excessive bleeding doesn't subside then the UFE would be considered a clinical failure.
You won't see the term "clinical failure rates" in medical literature, however. Instead, you'll see numbers that tout the statistics of how many women report "shrinkage" or reduced bleeding. Like this:
"...80-90% of all women undergoing UFE report...".
Sort of "reverse statistics" to get you to focus on the positive side of things. Here's the reality: 80-90% success rates invert to equate to 10-20% failure. Yep. 10-20% clinical failure rate. (Some IRs report 10-15% and others 15-20% -- statistics haven't really been pooled across the board yet with the results published.) The numbers look different to you now, don't they?
Here's something the numbers won't tell you:
Even with high clinical failure rates, women (even those who sustained clinical failure) are reporting that they would STILL choose UFE over hysterectomy or even myomectomy if they had to do it all over again.
Why is that? Why do women who've had "less than success" with their UFE still perceive it to be a better option? From my own personal experience, I would say it's because even though the procedure wasn't a complete success, it was enough to restore life back to an acceptable level of existence. And, at minimal surgical (technical) risk to me -- particularly compared to hysterectomy or even myomectomy.
Complications
Complications currently occur 1-2% of the time. Less than 1 in 200 women will acquire an infection that requires an immediate hysterectomy. Other items that contribute to the complication rate are:
- Finding that the woman has only a single uterine artery and the ovarian artery is feeding the fibroids (or, the uterine artery is feeding the ovary--the blood can actually flow in either direction). Doctors do one of two things in this case:
- Complete misembolization
of the ovarian artery. Results in menopause.
- Misembolization
of other areas that were not "targeted." Areas that would, oh
for example let's say, impact your buttocks or legs. None have been reported
to date--but it has occurred. What doctors do and what doctors "officially"
report are not always the same thing. Effects of misembolization are generally
temporary but can be quite serious, depending on what, exactly, the doctor
misembolized.
- Femoral
hematoma. A deep bruising of the puncture site (for arterial catheterization)
in the groin.
- Death.
While there have been no deaths reported in the United States from UFE,
there has been one death in England and possibly a second death in Italy
associated with UFE. Statistically, this represents a tiny fraction of the
number of women (over 6,500) who have undergone this procedure worldwide.
UPDATE
- Miscellaneous
side effects.
Doctors are still figuring these out as they are so infrequent that only
time and long range data collection will give them a more complete list.
Please ask your interventional radiologist for a more complete list of complication
possibilities during your initial appointment.
One of the side effects of UFE may well be some level of sexual dysfunction. (You can read about my own experience with this in My Journal.) If you are a woman who experiences uterine contractions or internal pelvic orgasms during sex and the blood flow to the cervix is altered because of uterine artery embolization, you may experience a loss of those contractions or internal orgasms. Although most women are reluctant to discuss this with their physician, I am aware of a number of cases (besides my own) where loss of internal orgasms and/or uterine contractions has, in fact, occurred. Several of us are nearing the one year mark post-UFE and have shown no signs of improvement. Clitoral orgasms and intensity of feeling in the vagina have also been reported as less intense with some women post UFE but in all cases that I am aware of to date these have returned to "normal" within 3 or 4 months. Until more women choose to openly discuss the issue of sex with their physicians both pre and post procedure we will not know how often sexual dysfunction actually occurs as a result of this procedure.
a) they partially embolize the ovarian artery (which may cause premature menopause) or
b) they go ahead and embolize the uterine artery and that's all (the fibroids continue to receive blood from the ovarian artery so the overall amount of "shrinkage" to the fibroids is reduced significantly--or, if the blood is actually flowing to the ovaries from the uterus, they've just shut off its blood supply--instant menopause).
|
Misembolization Misembolization is typically referred to as "non target embolization" in medical literature. I prefer the term "misembolization" but several IRs have pointed out that this implies there's been a "mis-take" when, in fact, there was simply an embolization of something non targeted and it could have been a mistake or simply materials going awry. It's a finer point to make and differentiate--one I think that is completely lost on most women. Hey--something got embolized that shouldn't have. End of story. Misembolization. |
History of UFE
There have been thousands of UFEs performed over the last 8 years for the specific treatment of uterine fibroids. Prior to that, uterine artery embolization (UAE) was reserved for women who began hemorrhaging following childbirth or after pelvic surgery (such as myomectomy).
UAE is a procedure that has been around for about 20 years and medical literature has detailed it as an effective means of stopping uncontrollable bleeding since 1979 or so. (Although the SCVIR recently changed the name of this procedure to represent it's specific treatment application for uterine fibroids, technically UAE and UFE are the same procedure.)
About 10 years ago (1989), an ob/gyn in Paris, France (Dr. Jacques-Henri Ravina) read the medical literature indicating that UAE was an effective means of stopping uncontrollable bleeding and decided to start using UAE PRE-myomectomy to cut down on the bleeding that patients would experience during the procedure. He was quite surprised to start finding women canceling out on their myomectomies. They no longer needed the myomectomy because their bleeding had subsided and their fibroids had actually begun to shrink.
From there, it took another 7 years before the procedure was introduced into the United States by Dr. Scott Goodwin at the UCLA Medical Center. Since introducing this procedure in 1996, there have been over 4,000 uterine fibroid embolizations performed in the United States. Nonetheless, it has been an uphill struggle to get gynecologists to recognize this promising procedure in the United States because it directly cuts into the revenue they currently receive from performing so many hysterectomies.
|
On Gynecologists and Money. . . Many a gynecologist has written to me indicating that they do not believe that gynecologists are refusing to refer for this procedure based on loss of revenue from not performing a hysterectomy. They are wholly unconvincing. Sorry guys. A woman's reproductive organs are clearly on the auction block of medicine in this country and the billion dollar HRT industry is standing in line right behind you encouraging you on. It is most definitely about money. Get busy doing some REAL research on sparing the uterus with uterine fibroid treatments and you might be a little more believable in your protests. No matter how many refinements of a hysterectomy you come up with, you need to understand that it is still a hysterectomy! Apparently that is a point missed by many gynecologists. |
The Doctors and Web Links
The following web links will lead you into a rather fascinating world of interventional radiology. You'll find an entirely different "breed" of doctors than the gynecologists you're probably accustomed to and you will be quite surprised at the information that many of them are choosing to present to women in an effort to ensure that you truly do understand all of the choices available for treatment of your uterine fibroids. For firsthand information about my own experiences with this choice, you can, of course, read My Journal. In addition, for ongoing discussions among women on this topic, please join us at the uterinefibroids chat group.
|
Link
|
Site
Name/Author
|
What
You'll Find
|
| www.auntminnie.com | Aunt Minnie | Radiology website/clearinghouse for news and information. "The first comprehensive community Internet site for radiologists and related professionals in the medical imaging industry." |
| www.fibroidtreatment.com | Scott C. Goodwin, MD | Comprehensive uterine fibroids treatment website brought to you by the Interventional Radiologist responsible for introducing Uterine Artery Embolization into the United States for the treatment of fibroids. |
| www.aafp.org/afp/20000615/ 3601.html |
Steve
Janney Smith, MD American Family Physician 2000;61:3601-7,3611-2. |
Uterine Fibroid Embolization. Cover article discussing UFE with comparitive analysis to other treatments currently available. |
| www.aafp.org/afp/ 20000615/editorials.html |
Anthony
R. Scialli, MD American Family Physician 2000;61:3559-3560. |
Is hysterectomy obsolete? An editorial from American Family Physician. |
| www.intelihealth.com/IH/ ihtIH/EMIHC000/333/ 333/261962 |
InteliHealth
Inc. The Associated Press news release |
1/10/00 Hope Offered Against Hysterectomy |
| starbulletin.com/1999/ 08/30/news/story2.html |
Honolulu
Star-Bulletin Helen Altonn |
8/30/99 Alternative to hysterectomy gains popularity here; Patients opting for new method call it fantastic, isle doctor says |
| www.wetreatfibroids.com/ | Dr.
George Fueredi Great Lakes Radiology Wisconsin |
Uterine
Artery Embolization: A Hysterectomy Alternative Also, <Focus On Your Body> FAQs. |
|
Before any link from Medscape.com will work, you must first register at www.Medscape.com. |
Medscape Women's Health 4(5), 1999 Suresh Vedantham, MD, Scott C. Goodwin, MD, Bruce McLucas, MD, Margaret Lee, MD, Rita Perrella, MD, Alice E. Forno, MD, and Mabel DeLeon |
Uterine Artery Embolization for Fibroids: Considerations in Patient Selection and Clinical Follow-up Discussion of uterine artery embolization as a noninvasive alternative to hysterectomy in the treatment of gynecologic bleeding for pre-menopausal women. |
| www.nytimes.com/library/ national/science/ 040699sci-fibroids-treatment.html |
NY Times: Susan Gilbert | 4/6/99 A Less Painful Way to Treat Fibroids |
| onhealth.com/ch1/briefs /item,38647.asp |
OnHealth
Network Company The New England Journal of Medicine |
3/23/99 Catheters Reduce Hysterectomies |
| cnn.com/HEALTH/9903/22/ fibroid.embolization/index.html |
CNN | 3/22/99 Little-used treatment effective against fibroid tumors |
| www.pslgroup.com/dg/EEC36.htm | Doctor's Guide to Medical and Other News | 3/22/99 SCVIR MEETING: Surgery-Sparing Treatment Successful For Treating Uterine Fibroids |
| www.radsci.ucla.edu:8000/ news/fibroids.html |
Dr. Scott
Goodwin, IR UCLA Department of Radiological Sciences |
New Treatment For Fibroids Can Alleviate The Need For Hysterectomy |
| www.scvir.org/fibroid/ | Society for Cardiovascular and Interventional Radiology | Uterine Fibroids: Symptoms and Diagnosis. Excellent informational web pages brought to you by the professional society of interventional radiologists who perform this procedure. |
| www.fibroids.org/ | Dr. Bruce
McLucas, UCLA Medical Group |
Home
page of Dr. Bruce McLucas: Detailed description of uterine embolization
and Dr. McLucas' special requirements for referral. (Note:
Dr. Scott Goodwin is not a staff member of Dr. McLucas' medical
firm. Although they have published papers together and worked together
in the past, Dr. McLucas now refers patients to an outpatient clinic for
UAE in Beverly Hills where he has purchased equipment and hired an IR
to perform UAE on all of his referred patients at that clinic.) Author's note: As a former patient of Dr. McLucas, I am providing this link for informational purposes only. Under no circumstances can I, personally, recommend Dr. McLucas. |
| www.fibroids.co.uk/thepaper.htm | Dr. W. J. Walker, Consultant Interventional Radiologist at the Royal Surrey County Hospital | Non-surgical treatment of fibroids in the UK by uterine artery embolisation - an alternative to hysterectomy, myomectomy and myolysis. |
| www.obgyn.net/ah/musings /musing_1.htm |
Dr. Francis Hutchins | Musings: The real scoop on uterine artery embolization. |
| www.drfibroid.com/ | Dr. Steven
Smith, IR Chicago Regional Center for the Nonsurgical Treatment of Uterine Fibroids |
Information on Fibroid Tumors and Alternatives to Hysterectomy |
| www.obgyn.net/women/features/ NS_Man_FIBROID.htm |
OBGYN.net Dr. Frank Vogel/Dr. Daniel Javit Lenox Hill Hospital Department of Radiology Division of Interventional Radiology |
Nonsurgical management of uterine fibroids. |
| www.lenoxhillhospital.org/ your_health/topic_detail.jsp?id=198 |
Lenox
Hill Hospital Dr. Daniel Javit Dr. Samuel I. Wahl |
The largest embolization center in New York City and in the greater New York region. |
| www.uhmc.com/fibroid.htm | The Fibroid
Embolization Center of the NY United Hospital Medical Center Dr. Carlos Forcade |
Fibroid embolization. . .a new treatment for uterine fibroids. |
|
www.diagnostic-imaging.com/ You must register
here: www.diagnostic- |
Tina
Barseghian SEPTEMBER 1997 DIAGNOSTIC IMAGING |
IMAGING NEWS Uterine fibroid embolization offers alternative to surgery: Interventionalists stop blood flow in uterine arteries. |
| www.fibroidoptions.com/ | Dr. James
B. Spies Georgetown Interventional Radiology Georgetown University Medical Center |
Uterine Artery Embolization (UAE) An alternative to surgery for patients with uterine fibroids |
| www.mirs.org/fibroids.htm |
MIRS Special Report Edward L. Siegel, MD, Department of Radiology, University of Kansas Medical Center |
New Treatment for Uterine Fibroids Avoids Surgery |
| www.mcrg.com/pe436.asp | Orlando Regional Medical Center Radiology Department | Explore the possibility of Uterine Artery Embolization (also called Uterine Fibroid Embolization) |
| www.ohsu.edu/dotter-fibroid/ | Dr. Robert
Andrews Dotter Institute Oregon Health Sciences University |
Uterine Fibroid treatment at OHSU. Excellent resource information for both patients and physicians. |
| www.raadocs.com | Radiology Associates of Atlanta | Interventional Radiologists in Georgia answer questions about UFE. |
| www.fibroidzone.com/ | Francis Hutchins, MD | The Fibroid Zone |
| www.fibroidcorner.com/ |
The Fibroid Corner |
Source of information on the diagnosis and management of uterine fibroids for both patients and health care providers. |
Home
| Choices | Diagnostics
| The Decision | Related
Health Issues | My Journal | Subscribe
| References
Medical Disclaimer | copyright
information ©1999-02 | send
Email
This page last updated Wednesday, April 10, 2002